What is Zika Virus?
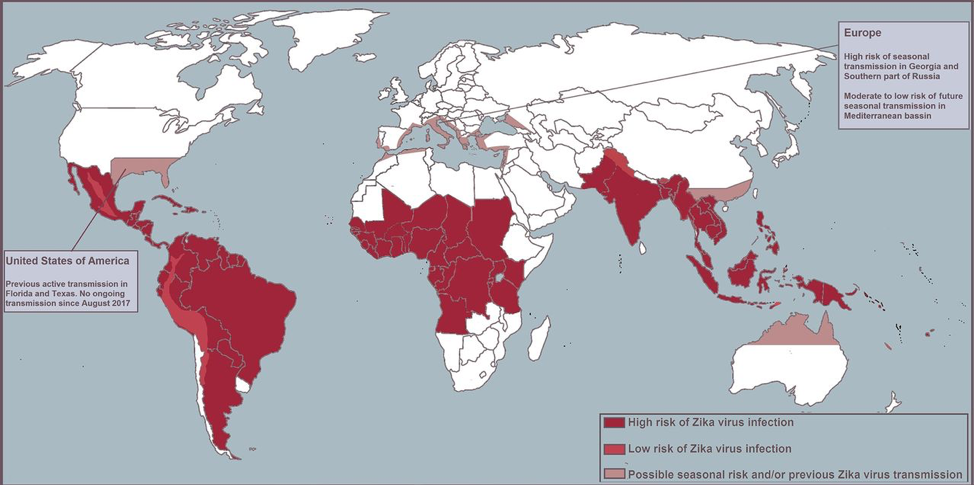
Zika virus is a flavivirus transmitted by the Aedes mosquitoes. Only 20% of adults infected will have clinical manifestations such as low-grade fevers, itchy rash, joint pain in the hands and feet, and eye inflammation. Current outbreaks are in the Americas, Caribbean, and Pacific, but cases have been seen around the world. In the USA transmission has occurred in Texas and Florida. While the primary mode of transmission is mosquito bites, vertical transmission to the baby from the mom in the uterus, during delivery, and potentially by breastmilk is possible. There is no vaccine to protect individuals from contracting the disease and current recommendations are to avoid areas with the virus that are below 6500 feet in altitude and using mosquito replant and protective clothing.
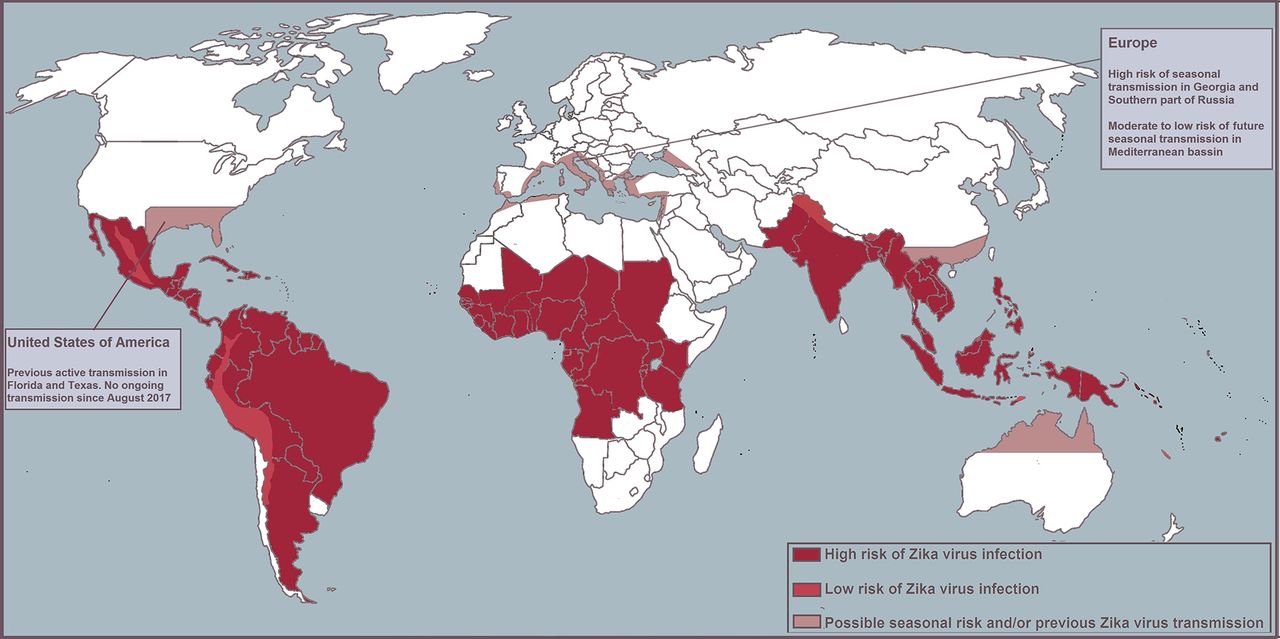
Image: Leonhard SE, Lant S, Jacobs BC, et al. Zika virus infection in the returning traveller: what every neurologist should know. Practical Neurology 2018;18:271-277.
What happens if my infant gets the Zika Virus?
When the fetus contracts the virus while still developing in the uterus, it can result in 3 major effects on the child’s brain- enlargement of the space occupying, fluid filled sacs called ventricles (33%), a small brain (24%), and calcification or hardening of the brain (27%). All of these have significant consequences on the brain development. It can also result in fetal loss (5-10%) (Vouga 2016). These estimates are from a review of 16 studies including 66 infants with confirmed zika virus. The risk of these complications is most common when the fetus contracts the virus during the 1st and 2nd trimesters. These complications are the reason the CDC recommends all pregnant women to avoid travel to areas with Zika virus.
Infants and children that acquire the Zika virus postnatally have a mild course similar to adults with fever, rash, and eye inflammation (Fleming-Dutra 2016). This is important because a breastfeeding mother with zika virus could potentially cause a postnatal infection in the infant. No developmental complications have been observed in children who are infected with the zika virus after birth (Karwowski 2016).
Should Moms who have zika virus still breastfeed?
Yes. Moms who have suspected or confirmed cases of zika virus are recommended by the world health organization to start breastfeeding within one hour of birth and continue exclusive breast feeding for at least 6 months according to the normal infant feeding guidelines. There are currently no reported cases of Zika virus being transmitted to infants through breastfeeding, but studies have showed the virus to be present in breast milk samples. Thus, breast milk is potentially infectious. Very little is known about how the virus in breast milk could infect the infant (World Health Organization 2016). In the two documented cases of neonates with confirmed cases of perinatally acquired zika virus, the infants had no long term complications. In fact, one was asymptomatic and the other had a rash and thrombocytopenia. The breastmilk of both mothers did contain Zika RNA, but due to the timing of infection these infants were likely infected before or during delivery (Besnard, 2016). In a case report of a 27-year-old female with confirmed zika virus, the lab found 35,000 RNA copies/ml in the mother’s blood serum on the third day and 850,000 RNA copies /ml in the breastmilk on the fourth day of being symptomatic from the zika virus. The infant was born on day zero, immediately breastfed, and remained clinically normal until discharge (Dupont-Rouzeyrol 2016). The difficulty of confirming viral transmission by breastmilk is also due to the asymptomatic nature of the acute virus (Colt 2017).
The benefits of breastfeeding for the infant include lower infectious morbidity and mortality, higher IQ, decreased risk of sudden infant death syndrome, and more. The benefits of breastfeeding for the mother include decreased risk of breast and ovarian cancer, decreased risk of diabetes, and more.
In conclusion, there still are no confirmed cases of infants being infected with Zika virus from contaminated breast milk. The infants that were infected postnatally with the virus suffered no long-term complications. There is overwhelming evidence of the benefits of breastfeeding. This means that the benefits of breastfeeding outweigh the risk of infection from the virus. Women should continue to breastfeed if they have a suspected or confirmed case of Zika virus.
Marcella Muysson MS3
Thomas W. Hale, Ph.D.
Teresa Baker MD
Infantrisk Center
January 22, 2018
References
Vouga, Manon, and David Baud. "Imaging of congenital Zika virus infection: the route to identification of prognostic factors." Prenatal diagnosis 36.9 (2016): 799-811.
Fleming-Dutra, Katherine E. "Update: interim guidelines for health care providers caring for infants and children with possible Zika virus infection—United States, February 2016." MMWR. Morbidity and mortality weekly report 65 (2016).
Karwowski, Mateusz P., et al. "Zika virus disease: a CDC update for pediatric health care providers." Pediatrics 137.5 (2016): e20160621.
World Health Organization. "Infant feeding in areas of Zika virus transmission." 2016. heep://www, who. int/elena/titles/guidance_summaries/zika/en (2017).
Dupont-Rouzeyrol, Myrielle, et al. "Infectious Zika viral particles in breastmilk." The Lancet 387.10023 (2016): 1051.
Besnard, M., et al. "Evidence of perinatal transmission of Zika virus, French Polynesia, December 2013 and February 2014." Eurosurveillance 19.13 (2014): 20751.
Colt, Susannah, et al. "Transmission of Zika virus through breast milk and other breastfeeding-related bodily-fluids: A systematic review." PLoS neglected tropical diseases 11.4 (2017): e0005528.